How to Redact PHI from Telehealth Session Recordings
by Ali Rind, Last updated: March 10, 2026 , ref:
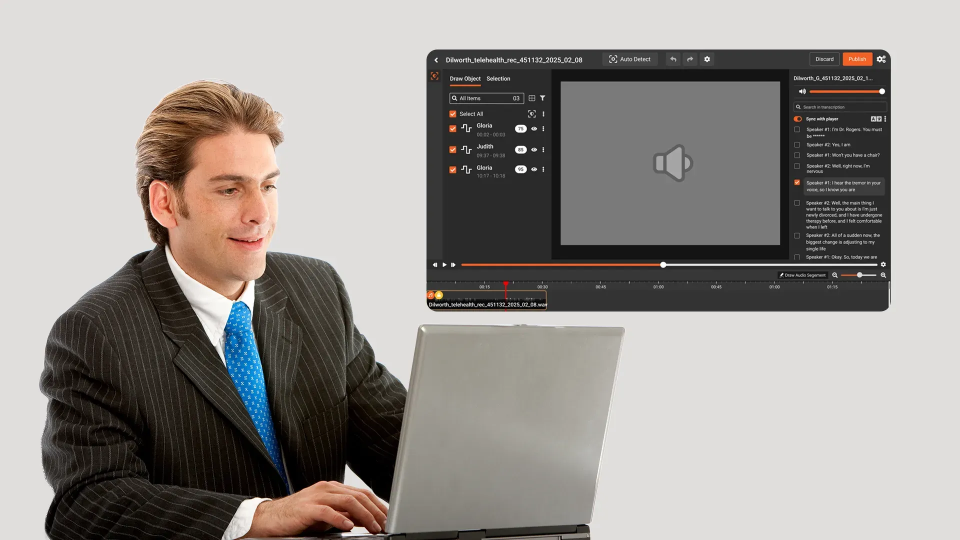
Telehealth adoption in behavioral health and broader healthcare has created a new category of PHI-rich records: video and audio recordings of virtual patient sessions. Whether it is an ABA therapy session conducted over Zoom, a psychiatric evaluation via a telehealth platform, or a routine primary care follow-up, these recordings capture PHI in ways that traditional paper records never did.
When organizations need to share, store, or review these recordings for supervision, quality assurance, training, legal requests, or insurance audits, they must redact PHI from telehealth recordings before any disclosure. The challenge is that video and audio contain PHI in multiple layers, and removing it requires more than simple text redaction.
What PHI Appears in Telehealth Session Recordings
Telehealth recordings capture sensitive information across visual, auditory, and metadata layers simultaneously. Understanding where PHI hides is the first step toward effective redaction.
Visual PHI in the video stream. Patient faces are the most obvious visual identifier, but telehealth recordings capture much more. Backgrounds may reveal prescription bottles, medical devices, or personal documents. Screen shares during consultations may display patient charts, lab results, or insurance details. Name placards or display names on the video call interface often show the patient's full name.
Spoken PHI in the audio stream. Conversations between clinicians and patients naturally include PHI: the patient's name, date of birth, medication names and dosages, symptoms, diagnoses, treatment history, and insurance details. In behavioral health sessions specifically, therapists may reference family members by name, discuss specific behavioral incidents at school or home, and review treatment goals tied to identified conditions.
Embedded metadata. Recording files often carry metadata including the date and time of the session, participant names, email addresses used to join the call, and device identifiers. This metadata may not be visible during playback but is embedded in the file and accessible to anyone who inspects the file properties.
On-screen text overlays. Many telehealth platforms display participant names, timestamps, and closed captions during the session. If the recording captures these overlays, they become additional PHI that needs redaction even if the underlying audio is also being processed.
HIPAA Requirements for Recorded Telehealth Sessions
HIPAA does not prohibit recording telehealth sessions, but it imposes strict requirements on how those recordings are handled. Any recording containing individually identifiable health information qualifies as PHI and is subject to the Privacy Rule and Security Rule. For a full breakdown of how these rules apply to video content, see HIPAA-Compliant Video Platform for Secure Health Data.
Minimum necessary standard. When sharing a recorded session for a purpose like clinical supervision or quality review, organizations must disclose only the minimum PHI necessary. If the reviewer does not need to know the patient's identity, the recording must be redacted before sharing.
Business associate agreements. If recordings are stored on a third-party platform or processed by an external redaction service, a Business Associate Agreement (BAA) must be in place. This applies to cloud storage providers, transcription services, and redaction software vendors.
Breach notification obligations. An unredacted recording shared without authorization constitutes a potential breach. Under the HIPAA Breach Notification Rule, organizations must notify affected individuals, the Department of Health and Human Services, and in some cases the media, depending on the scale of the breach.
The stakes are significant. More than 540 healthcare organizations experienced data breaches in 2023 alone. Behavioral health records carry particular sensitivity because they document mental health conditions, substance abuse treatment, and developmental disabilities, all categories that carry social stigma and heightened privacy expectations.
Why Manual Redaction Fails for Video and Audio
Manual redaction is impractical for telehealth recordings for reasons that go well beyond time constraints.
Multi-layer complexity. A single telehealth recording contains PHI in the video feed (faces, screen content, backgrounds), the audio track (spoken names, diagnoses, medications), and embedded metadata. Manual redaction would require a person to process each layer separately: blurring video elements frame by frame, muting or bleeping audio segments, and stripping metadata fields.
Time and labor costs. Manually redacting one hour of video can take 4 to 8 hours of analyst time, depending on the density of PHI and the number of redaction passes required. For a behavioral health practice recording 20 to 50 telehealth sessions per week, manual redaction is not operationally feasible. Small compliance teams face this challenge acutely, as explored in Automate PHI Redaction for Small Healthcare Compliance Teams.
Audio PHI is invisible to the eye. Unlike visual PHI that can be spotted on screen, spoken PHI can only be identified by listening to the entire recording in real time. Manually flagging every instance where a patient name, medication, or diagnosis is spoken is exhausting and error-prone.
No standardized process. Without automated tooling, each staff member applies their own judgment about what constitutes PHI in a recording. This inconsistency creates compliance gaps that are difficult to detect until an audit or breach investigation reveals them.
How Automated Video and Audio Redaction Works
Automated redaction software uses AI models trained to detect and redact PHI across video, audio, and document formats simultaneously. Here is how the process works for telehealth recordings.
Face and object detection. AI models identify faces, persons, and other visual identifiers in the video stream. Detected elements are tracked across frames and redacted using blur, pixelation, or black box overlays. This handles patient faces, bystanders in the background, and any other visually identifying content.
Spoken PII detection and removal. Natural language processing (NLP) models analyze the audio track to identify spoken PHI categories, including names, dates of birth, addresses, phone numbers, Social Security numbers, and medical terms. Detected segments are automatically muted or replaced with a bleep tone. Support for 82 or more languages ensures that multilingual patient populations are covered. Learn more about how this works in Spoken PII Redaction with VIDIZMO Redactor.
On-screen text and document detection. If the recording includes screen shares or on-screen text overlays (participant names, chat messages, clinical documents), optical character recognition (OCR) and text detection models identify and redact this content within the video frames.
Metadata stripping. Automated tools remove or redact embedded metadata fields like participant names, email addresses, and session identifiers from the recording file itself.
Configurable confidence thresholds. Not every AI detection is equally confident. Automated redaction tools allow compliance teams to set confidence thresholds. Detections above the threshold are automatically redacted. Those below it are flagged for human review, ensuring that uncertain cases get manual attention without requiring staff to review the entire recording.
Audit trail generation. Every detection and redaction action is logged with timestamps, confidence scores, and the identity of the person who initiated or approved the process. This documentation is essential for demonstrating HIPAA compliance during audits.
For a broader look at how AI-powered redaction handles healthcare video content across formats, see Healthcare Data Redaction Software by VIDIZMO Redactor.
Building a Telehealth Redaction Workflow
Healthcare organizations recording telehealth sessions should build redaction into their standard operating procedures rather than treating it as an afterthought. For organizations using HIPAA-compliant video platforms, capabilities like automated redaction, access controls, and audit logging should already be part of the infrastructure. See HIPAA-Compliant Telehealth Platforms 101 for a detailed overview of what a compliant platform should include.
Define sharing scenarios. Identify every situation where a telehealth recording might be shared: clinical supervision, peer review, quality assurance, insurance audits, legal requests, training programs, and research. Each scenario may require a different redaction policy.
Set up automated redaction policies. Configure redaction rules that match your sharing scenarios. A training use case might require full face and name redaction, while an insurance audit might only require removal of non-relevant third-party PHI. Policy-based automation ensures the right redaction is applied every time without manual decision-making. For guidance on building these policies correctly, Video Redaction Best Practices is a useful reference.
Process recordings promptly. Do not let unredacted recordings accumulate. Schedule regular redaction runs, ideally within 24 to 48 hours of the session, to minimize the window during which unredacted files exist in storage.
Preserve originals securely. Redacted copies should be the default for sharing. Unredacted originals must be stored with appropriate access controls, encryption, and retention policies. The original is essential for clinical continuity and as a legal reference.
Consider AI input risks. If your organization uses AI tools to summarize or analyze session recordings, redacting PHI before the content reaches any AI platform is critical. Feeding unredacted recordings into external AI systems creates additional compliance exposure. For more on this risk, see LLM Redaction Risk: Redact Before Using Any AI Platform.
Key Takeaways
- Telehealth recordings contain PHI across four layers: video (faces, screens), audio (spoken names and diagnoses), metadata (participant emails, session IDs), and on-screen text overlays.
- HIPAA requires minimum necessary disclosure, meaning recordings must be redacted before sharing for supervision, audits, or training.
- Manual redaction of video and audio is operationally impractical, often taking 4 to 8 hours per hour of footage.
- Automated redaction uses AI to detect and remove PHI across all layers simultaneously, with configurable confidence thresholds for human oversight.
- Building redaction into standard workflows with scheduled batch processing reduces compliance risk and operational burden.
Protecting Patient Privacy in the Age of Virtual Care
Telehealth has made healthcare more accessible, but it has also created a new class of PHI-rich records that organizations were not designed to manage. Recorded sessions capture everything, from a patient's face to their spoken medical history, in a single file. The organizations that treat redaction as a core part of their telehealth workflow, rather than an afterthought, will be best positioned to meet HIPAA requirements while continuing to benefit from recorded session data for training, quality improvement, and clinical oversight.
Protect patient privacy in telehealth recordings with AI-powered PHI redaction. Contact us today to see how VIDIZMO Redactor can help you automatically detect and remove sensitive information from video and audio.
People Also Ask
PHI can be removed from telehealth recordings using automated redaction tools that detect and blur faces, mute spoken identifiers, redact on-screen text, and strip metadata. AI-powered redaction software can process video, audio, and text simultaneously to ensure HIPAA-compliant sharing.
Yes. Telehealth recordings usually contain identifiable health information such as patient faces, names, diagnoses, and treatment discussions. Because they include protected health information, they must be stored, accessed, and shared in compliance with HIPAA regulations.
Telehealth recordings may contain PHI in several forms including patient faces, spoken names, diagnoses, medications, dates of birth, on-screen medical records, chat messages, and embedded metadata such as participant emails or session IDs.
Yes, but only after PHI is properly redacted. HIPAA’s minimum necessary rule requires removing identifiable patient information before recordings are used for training, quality assurance, research, or clinical supervision.
Manual redaction is difficult because PHI exists across multiple layers such as video frames, audio conversations, on-screen text, and metadata. Reviewing and editing each layer manually is time-consuming and prone to human error.
AI-powered video redaction tools can automatically detect faces, identify spoken personal information, recognize text through OCR, and remove sensitive metadata. These tools significantly reduce the time required to redact telehealth recordings.
About the Author
Ali Rind
Ali Rind is a Product Marketing Executive at VIDIZMO, where he focuses on digital evidence management, AI redaction, and enterprise video technology. He closely follows how law enforcement agencies, public safety organizations, and government bodies manage and act on video evidence, translating those insights into clear, practical content. Ali writes across Digital Evidence Management System, Redactor, and Intelligence Hub products, covering everything from compliance challenges to real-world deployment across federal, state, and commercial markets.
Jump to
You May Also Like
These Related Stories
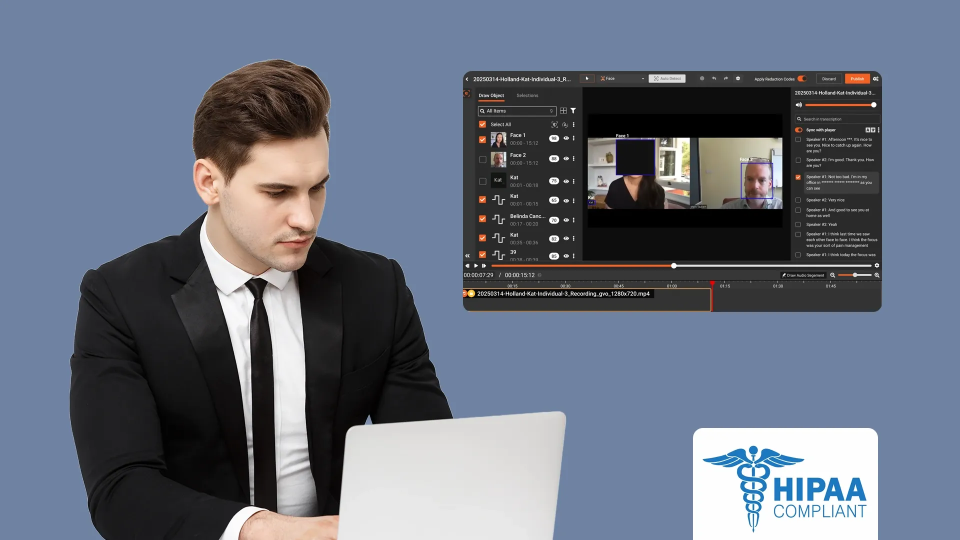
How to Redact PHI from SaaS Product Demo Videos

HIPAA-Compliant Video Redaction Tools for Healthcare




No Comments Yet
Let us know what you think